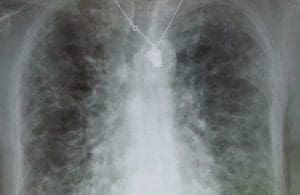
Idiopathic pulmonary fibrosis x-ray courtesy of Wikimedia Commons.
This September is Pulmonary Fibrosis Awareness Month, which the Pulmonary Fibrosis Foundation (PFF) and allies have launched to educate the public about the disease family. Involving scarring of the lungs, pulmonary fibrosis gradually robs the breath from patients it affects.
Some 250,000 Americans live with idiopathic pulmonary fibrosis, according to PFF.
At present, two drugs are available to treat the condition in the U.S., but pulmonary fibrosis remains an active focus area for drug developers.
Given that September is Pulmonary Fibrosis Awareness Month, the anniversary of the September 11 attacks also can serve as a reminder of the impact of interstitial lung disease. “Lots of lung disease has occurred in the first responders of the World Trade Center,” said Dr. Joyce Lee, a senior medical advisor for the Pulmonary Fibrosis Foundation. While there is “still a lot to learn from the lung disease” that emerged from those at Ground Zero, it seems likely that the inhaled particulate matter at the site led to both acute and long-term consequences.
A 2019 study in the International Journal of Environmental Research and Public Health explored the connection between dust from the trade center attacks and pulmonary fibrosis.

Joyce Lee, MD
Dr. Joyce Lee is an associate professor, medicine specializing in pulmonary sciences and critical care
The pandemic has been hard on patients with pulmonary fibrosis and other types of interstitial lung disease. Some patients with the conditions have faced limited access to healthcare and, in some parts of the U.S., difficulty in finding supplemental oxygen.
And COVID-19 itself, like other viral respiratory infections, has worsened symptoms for patients with pre-existing lung disease. The possibility that COVID-19 can lead to interstitial lung disease is “an area of active research,” said Lee, who is also a professor specializing in pulmonary sciences and critical care at the University of Colorado. “We know bad viral infections of the chest can lead to scarring of the lungs, and, for most patients, that’s a non-progressive process,” Lee said.
In any event, the pandemic has brought renewed attention to pulmonary fibrosis and interstitial lung disease, but most of the public is unaware of the condition. A recent survey from the Pulmonary Fibrosis Foundation found that nearly nine out of 10 Americans were not familiar with PF symptoms.
“A lot of education” is still required, Lee said.
In addition to educational campaigns for the broader public, physicians specializing in treating the condition should also reach out to other physicians, including primary care doctors and other pulmonologists, to “make sure it’s on their radar as well,” Lee said.
Improving awareness through education could lead to earlier diagnosis. According to a BMJ article, diagnosing the condition can often take a year or longer.
Part of the challenge of initial diagnosis is that a range of diseases can initially present similarly to pulmonary fibrosis. There are, however, “certain medical history elements, certain medical problems, medications and physical exam findings that can raise your suspicion even in the earlier symptom phase,” Lee said.
Two factors that could improve the treatment landscape for the condition include continued investment from drug developers and increased collaboration among medical experts. In her work at the University of Colorado, Lee is an advocate for a multi-disciplinary approach to studying the disease. At the university, colleagues in pulmonology, rheumatology, radiology and pathology collaborate to deepen their respective understanding of pulmonary fibrosis and the broader category of interstitial lung disease. “We’ve learned over time that individual physicians working independently is not as good as [working across disciplines collaboratively],“ Lee said.
Filed Under: clinical trials, Drug Discovery, Pulmonology





Tell Us What You Think!
You must be logged in to post a comment.