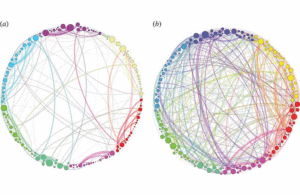
Communication between brain networks in people given psilocybin (right) or a non-psychedelic compound (left). [Image courtesy of Wikimedia Commons]
But while traditional psychedelics like psilocybin may have broad potential, making effective therapeutic use of them at scale is likely to be challenging in the near term, said psilocybin advocate Derek Chase, who has experience working in the pharmaceutical, cosmetic and cannabis industries.
“The mental health segment needs to be readdressed from the ground up” to make the most of psychedelics, Chase said. With psychedelics, the mental health industry should strive to find a “true linking of medication with therapy.”
Psychedelics such as psilocybin should have a “service element,” Chase said. He points to well-monitored psychedelic retreats as a promising model to unlock the therapeutic promise of psychedelics without the confines of traditional mental-health treatment.
Conversely, psychiatrists such as Columbia University professor Dr. Jeffrey Lieberman have called for firmer data on the therapeutic efficacy of psychedelics before endorsing them. Lieberman has also called for safeguards to limit potential harm related to the therapeutic use of psychedelics.
“Should the mind-bending properties of psychedelics prove to be the panacea their proponents professed, informed consent and safety standards must be established,” Lieberman wrote in NEJM last year.
Some trained mental health professionals have backed psychedelic-assisted psychotherapy, which weaves a psychedelic compound into the psychotherapeutic process.
The London-headquartered company Compass Pathways has developed a therapist training program based on feedback psychologists, psychiatrists and psychdelic therapy researchers. The company stipulates that all of the therapists involved in its clinical trials be mental health professionals.
Chase fears that a template-based traditional mental-health approach to incorporating psychedelics into therapy may have limited efficacy. “If you’re truly mentally ill, you shouldn’t have to rely on a cookie-cutter approach that fits into your daily life,” he said.
The psychedelic drugs market could be worth $6.85 billion by 2027, according to Data Bridge Market Research.
While psychedelics aren’t a “magic pill,” they could hold promise for many people with depression, anxiety or other conditions who are willing to take time to explore them in the right setting, Chase said. Examples may be a weekend- or week-long retreat staffed with experts.
Chase also calls for incorporating mindfulness with psychedelic-based therapy. Mindfulness is currently popular as an adjunct to cognitive therapy, which can complement drug therapies that treat depression and anxiety.
While meditation and other mindfulness-based activities can lead to significant mental health benefits over time, “psychedelics really increase the rate at which you can experience these moments of clarity,” Chase said. “But on the flip side, you’re not necessarily going to integrate those experiences and have lasting improvements” with psychedelics alone.
Chase says meditation can help patients before beginning a psychedelic regimen and during therapy. “A lot of people simply want to pop a pill like a pharmaceutical company would recommend,” Chase said.
The growing cultural acceptance of cannabis in North America could be a blessing and a cure for legitimizing psychedelics. But unfortunately, many people continue to view cannabis as a “party drug or escapist drug rather than a therapeutic drug,” Chase said. “That’s partly because of legalization and the resulting Cheech and Chong approach to marketing.”
Researchers exploring the therapeutic potential of psychedelics could help by continuing to gather more-rigorous data on the compounds’ therapeutic potential.
A recent study published in the Journal of Psychopharmacology concluded that “psilocybin mushrooms are a relatively safe drug, with serious incidents rare and short-lasting.”
“We look at psilocybin as a step up in terms of legitimacy within the eyes of the consumers,” Chase said.
In Canada, Numinus Wellness Inc. (TSXV:NUMI; OTCPK:LKYSD) is the first publicly-traded company to win a license from Health Canada related to psilocybin.
Chase says Oregon could also play a vital role in legitimizing the therapeutic use of psilocybin. The state is slated to widely legalize psilocybin services in 2023 after it passed Ballot Measure 109 in November 2020.
“We’re watching very closely from the draft rulings perspective to understand how they’re going to be regulating and luckily, it sort of bypasses the current medical system,” Chase said. “It’s its own insulated program that requires training and licensure. We’re really actually excited what we’ve seen from out of Oregon so far.”
Filed Under: Psychiatric/psychotropic drugs





Tell Us What You Think!
You must be logged in to post a comment.